KEY POINTS
- Updated medical standards recommend starting cholesterol management much earlier in a patient’s life.
- Heart associations now advocate for more aggressive “bad” cholesterol targets to prevent cardiovascular events.
- The new framework emphasizes personalized risk assessments instead of relying solely on age-based metrics.
The American Heart Association and the American College of Cardiology have released updated clinical guidelines. These new standards fundamentally change how medical professionals approach cholesterol management for various age groups. The primary focus shifts toward proactive prevention and significantly lower target levels for high-risk patients.
Health experts now suggest that interventions should begin much earlier than previously recommended. Research indicates that cumulative exposure to high cholesterol over decades increases the risk of heart disease. By addressing these levels in early adulthood, patients can potentially avoid long-term damage to their arteries.
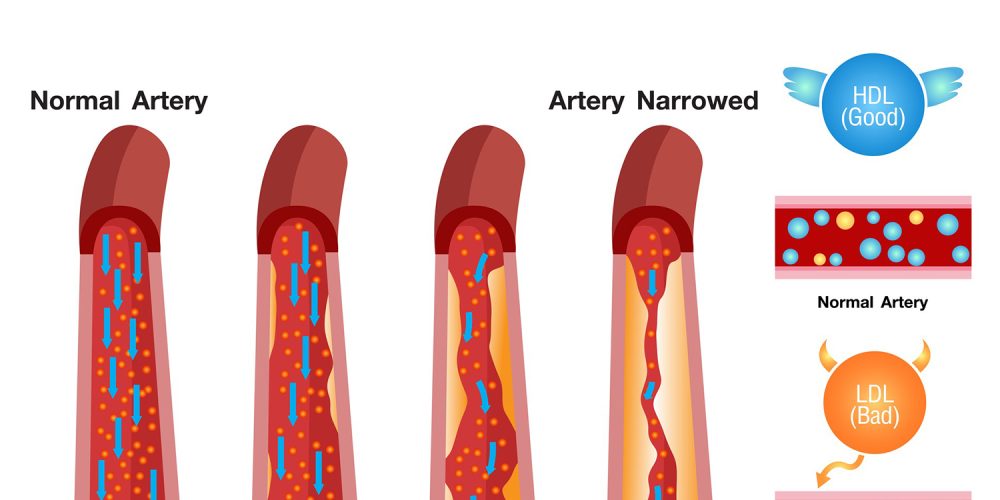
The updated guidelines place a heavy emphasis on Low-Density Lipoprotein, commonly known as “bad” cholesterol. For individuals at the highest risk of heart attack or stroke, the recommended threshold has dropped. Doctors are now encouraged to push these levels lower than the previous standard of 70 mg/dL.
Personalized risk assessment serves as a cornerstone of the new medical strategy. Rather than using a one-size-fits-all approach, physicians must consider a wide array of “risk enhancers.” These include family history, chronic kidney disease, and specific inflammatory conditions like rheumatoid arthritis.
The use of coronary artery calcium (CAC) scores has also gained more prominence in these updates. This non-invasive scan helps doctors determine the actual buildup of plaque within the heart’s arteries. If the score is zero, some patients may be able to delay starting statin medications.
Lifestyle modifications remain the first line of defense in the new cholesterol management hierarchy. The guidelines reinforce the importance of a heart-healthy diet, regular physical activity, and weight management. However, the report acknowledges that many patients will still require pharmaceutical assistance to reach their targets.
Statin therapy remains the primary medication choice for lowering cholesterol levels effectively. For patients who do not reach their goals with statins alone, the guidelines suggest adding non-statin therapies. These secondary options include ezetimibe and PCSK9 inhibitors for those with the most stubborn cases.
The committee also highlighted the importance of clinician-patient shared decision-making. This process ensures that patients understand their specific risks and the benefits of various treatment options. Clear communication helps improve adherence to long-term medication schedules and lifestyle changes.
Special attention is now given to younger populations and diverse ethnic groups. The updated data shows that certain populations face higher cardiovascular risks at lower cholesterol levels. This nuanced view allows for more equitable and effective healthcare delivery across different communities.
By implementing these aggressive new targets, health organizations aim to reduce the global burden of heart disease. Cardiovascular issues remain a leading cause of death worldwide, often due to unmanaged cholesterol. These guidelines provide a clear roadmap for both doctors and patients to improve long-term outcomes.
Regular screening is essential for the success of this new preventative model. Adults should discuss their lipid profiles with their healthcare providers during annual checkups. Early detection and consistent management are the most effective tools for maintaining a healthy heart.