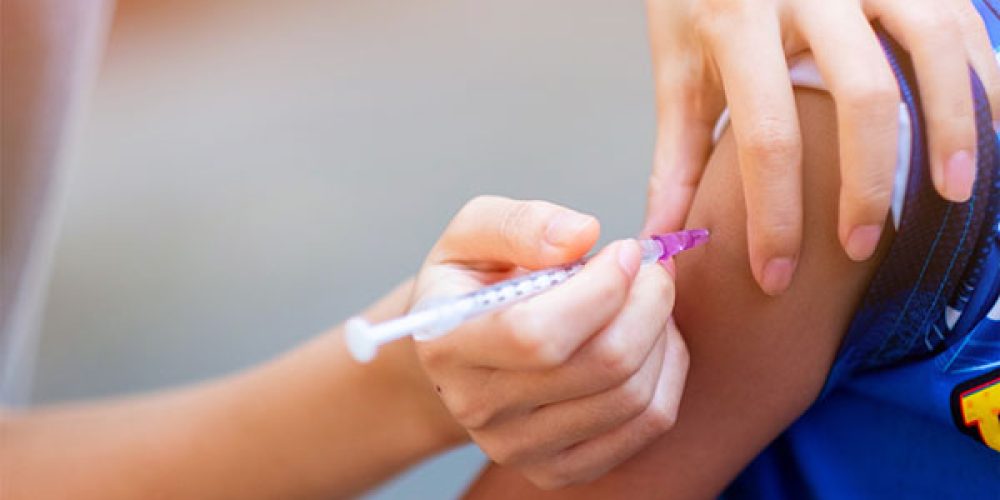
When it comes to getting a vaccine in the upper arm, the length of the needle can make a big difference. Health specialists are increasingly warning that using the wrong needle size — too short or too long — may reduce effectiveness or increase the risk of complications. Ensuring proper needle length helps deliver the vaccine into the muscle where it should go, avoiding under- or over-penetration.
Vaccines are often administered into the deltoid muscle of the shoulder. If the needle is too short, the vaccine may end up in fat or connective tissue instead of muscle. That can limit how well the immune system responds. On the flip side, a needle that’s too long could hit bone or injure nearby tissues, which can cause pain or even damage.
Medical experts now emphasize matching needle length to a patient’s body type. For many adults, a standard 1-inch (25 mm) needle works fine. But for people with more body fat in the arm, a longer 1.5-inch (38 mm) needle may be safer to ensure the injection reaches the muscle. For children and teens, or slim adults, shorter needles may suffice — but only if they allow safe muscle penetration.
National and global immunization guidelines already highlight the importance of needle size. However, studies show real-world vaccination practices sometimes fall short. Some clinics continue to standardize needle use for all patients, failing to adjust based on arm size or gender. That may explain why certain individuals report weaker immune responses or more localized side effects after vaccination.
Correct needle use also matters for reducing injection-site adverse events. Proper intramuscular delivery helps ensure the vaccine spreads correctly inside muscle tissue; when the vaccine is placed too shallow, it can irritate fatty tissue and cause soreness, lumps, or even suboptimal immunity. For intramuscular vaccines, that can undermine what the shot was meant to accomplish.
Healthcare providers can improve outcomes by using a simple measurement method before injecting. They can estimate tissue depth by gently pinching the patient’s upper arm to gauge fat thickness. If pinching lifts more than about 1 cm of tissue, a longer needle may be needed. Medical staff should also consider patient factors such as age, sex, body mass index (BMI), and muscle mass when selecting needle size.
In settings where many patients need vaccination — from local clinics to mass immunization campaigns — adopting flexible needle-length protocols can help. Clinics should stock different needle sizes, train staff accordingly, and consider document-based guidance rather than one-size-fits-all practices. That shift can help maximize vaccine effectiveness, especially in large-scale efforts like flu campaigns or childhood immunization drives.
Some experts also recommend further research. They say large-scale studies should evaluate whether individualizing needle length leads to better immune response rates and fewer side effects. In addition, public health agencies might consider updated training for all vaccinators, emphasizing needle selection as part of overall injection safety protocols.
For individuals receiving vaccines, awareness can help too. People can ask their healthcare provider whether the selected needle suits their build — especially if they are overweight, very lean, or elderly. Clear communication about these small but important decisions can improve confidence and outcomes.
In short: needle length isn’t trivial. Ensuring injections penetrate muscle appropriately can make vaccines safer and more effective. As vaccination programs continue worldwide, attention to this detail may help improve public health outcomes one shot at a time.