KEY POINTS
- Scientists have identified specific blood biomarkers linked to gut bacteria that can forecast cognitive decline years before symptoms appear.
- The breakthrough suggests that the “gut-brain axis” plays a more significant role in neurological health than previously understood.
- Early screening via this non-invasive method could revolutionize preventative care and personalized treatment plans for aging populations.
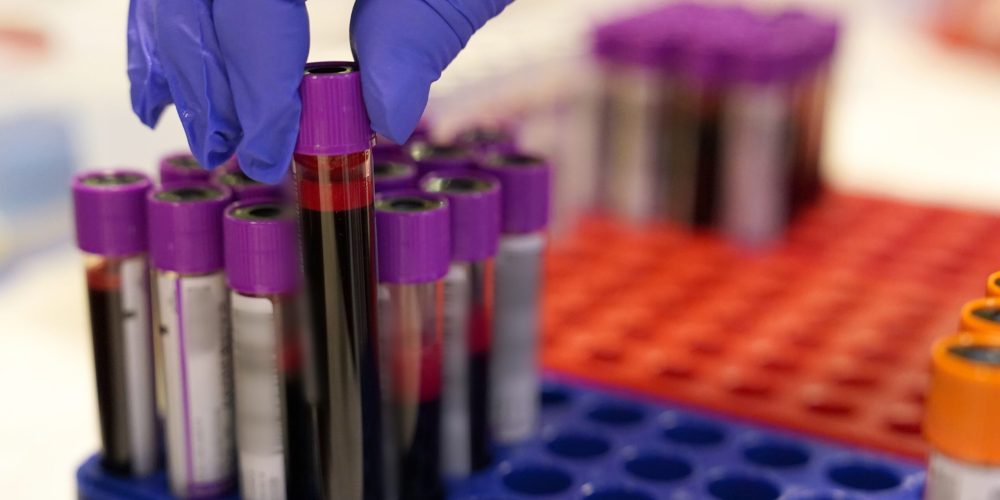
A revolutionary new blood test may soon allow doctors to predict a patient’s risk of developing dementia by analyzing chemical signals sent from the digestive system. By identifying specific metabolites produced by gut bacteria, researchers have found a way to spot the warning signs of cognitive decay long before memory loss or confusion sets in. This discovery offers a significant leap forward for proactive medicine, shifting the focus from managing late-stage symptoms to early intervention.
What You Need to Know
Dementia remains one of the most significant challenges for modern healthcare, affecting millions of families across the globe. Traditionally, diagnosing conditions like Alzheimer’s disease has relied on cognitive assessments or expensive brain imaging that only detects damage once it has already occurred. The medical community has spent decades searching for a “biological window” that would allow for earlier detection, and recent focus has increasingly turned toward the complex relationship between the intestines and the brain.
The “gut-brain axis” refers to the bidirectional communication network that links the enteric nervous system in the gut with the central nervous system in the brain. Scientists have long suspected that imbalances in the microbiome—the trillions of microbes living in the digestive tract—can trigger systemic inflammation. This inflammation is believed to contribute to the breakdown of the blood-brain barrier, eventually leading to the protein buildup and neuronal death associated with cognitive impairment.
This new research highlights specific biomarkers in the blood that serve as a bridge between these two systems. Instead of looking for brain-derived proteins, the test identifies small molecules that are generated in the gut and then travel through the bloodstream. When these molecules appear in certain concentrations, they act as a red flag for the neurological changes that precede clinical dementia.
Predicting Cognitive Decline Through Gut Health
The development of this diagnostic tool involved a meticulous study of how our metabolic byproduct affects brain longevity. Researchers analyzed blood samples from large cohorts over several years, correlating the levels of gut-derived metabolites with subsequent performance on memory and problem-solving tests. The results were striking: individuals with specific “gut signatures” were significantly more likely to experience a rapid drop in mental acuity as they aged.
Specifically, the study points to the role of certain inflammatory markers that originate in the digestive tract. When the gut microbiome becomes imbalanced—a state known as dysbiosis—it produces toxins that can enter the circulatory system. These toxins don’t just affect digestion; they appear to exacerbate the aging process of the brain. The new blood test effectively measures this “leakage” and its impact on the body’s internal environment.
The timeline for this diagnostic capability is what truly excites the medical field. Current models suggest that the test could identify high-risk individuals up to a decade before they would typically receive a formal diagnosis. This provides a massive head start for lifestyle modifications, such as dietary shifts and targeted probiotic therapies, which have shown promise in slowing the progression of neurodegenerative diseases.
Furthermore, the simplicity of a blood draw makes this an accessible option for routine check-ups. Unlike lumbar punctures or PET scans, which are invasive and costly, a metabolic blood panel could be integrated into annual physicals for adults over 50. By making early detection a standard part of geriatric care, the healthcare system could move toward a more sustainable model of managing the aging process.
Why This Matters
For the average American, this development represents a potential shift in how we approach the “inevitability” of aging. The U.S. healthcare system currently spends billions of dollars on late-stage memory care, a burden that often falls on family members who must leave the workforce to provide support. A reliable, early-warning system could significantly reduce these long-term costs by keeping the aging population independent for longer periods, fundamentally changing the economic landscape of senior living and insurance.
On a global scale, particularly in aging nations like Sweden and Ireland, the integration of gut health into neurological screenings could lead to new dietary guidelines as part of public health policy. If certain fermented foods or fiber-rich diets are proven to influence the biomarkers found in this blood test, we may see a rise in “neuro-protective” nutrition programs. This empowers individuals to take control of their cognitive destiny through measurable, science-backed lifestyle choices rather than waiting for pharmacological solutions that are often out of reach or come with significant side effects.
NCN Analysis
The link between gut health and the brain is no longer a fringe theory; it is becoming a cornerstone of 21st-century diagnostics. At NextClickNews, we anticipate that this blood test will be the first of many tools that look at the body as an integrated system rather than a collection of isolated organs. The next logical step for the pharmaceutical and wellness industries will be the development of “psychobiotics”—probiotics specifically designed to target the biomarkers identified in this study to preserve mental function.
However, readers should remain cautious about the timeline for widespread clinical availability. While the science is sound, regulatory approval and the standardization of what constitutes a “healthy” gut signature across diverse populations will take time. We should watch for upcoming longitudinal trials that test whether changing the gut microbiome actually reverses the biomarker levels and, subsequently, the risk of decline. If those trials succeed, the definition of “brain food” will change forever.
The ability to look into a vial of blood and see the future of a person’s memory is a powerful prospect that brings us one step closer to a world without the shadow of dementia.
Reported by the NCN Editorial Team