KEY POINTS
- New clinical research highlights a direct physiological link between untreated obstructive sleep apnea (OSA) and an increased risk of chronic heart failure and stroke.
- Cardiologists are now recommending sleep studies as a standard diagnostic tool for patients showing early signs of hypertension or irregular heart rhythms.
- Consistent use of CPAP therapy or oral appliances has been shown to reduce cardiac strain by stabilizing oxygen levels and lowering nighttime blood pressure.
The medical community is issuing a vital reminder that the quality of your sleep is a primary pillar of cardiovascular wellness. According to a report featured on Yahoo News, obstructive sleep apnea—a condition where breathing repeatedly stops and starts during sleep—is much more than a cause of loud snoring or daytime fatigue. It is a significant, often “silent” driver of heart disease. When breathing is interrupted, oxygen levels in the blood drop sharply, triggering a “fight or flight” response that spikes adrenaline and puts immense pressure on the heart and blood vessels.
Over time, this repetitive nightly stress leads to structural changes in the heart. Specifically, untreated apnea is a major contributor to atrial fibrillation (Afib) and resistant hypertension, where blood pressure remains high despite medication. For individuals already managing heart conditions, failing to address sleep disruptions can negate the benefits of other treatments. Specialists emphasize that the heart never truly “rests” if the body is constantly struggling for air, leading to a state of chronic inflammation that accelerates the hardening of the arteries.
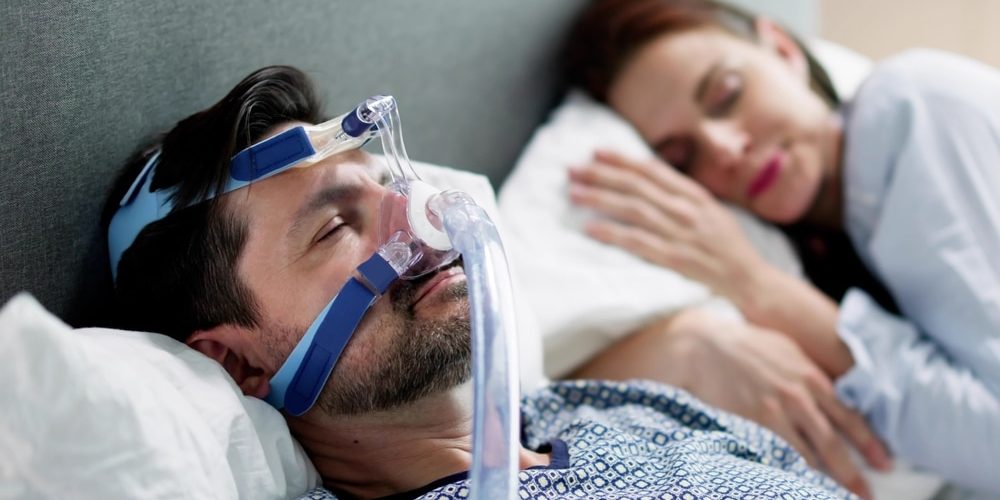
Fortunately, the path to protecting your heart through better sleep has become more accessible. Modern diagnostic tools, including at-home sleep tests, allow patients to identify breathing issues without a mandatory overnight stay in a clinical lab. Once diagnosed, treatments like Continuous Positive Airway Pressure (CPAP) machines or custom-fitted dental devices act as a mechanical “internal splint,” keeping the airway open. Clinical data shows that patients who consistently use these therapies see a marked improvement in heart rate variability and a reduction in the long-term risk of cardiovascular events.
Beyond high-tech machinery, lifestyle modifications remain a critical secondary defense. Weight management, side-sleeping techniques, and avoiding alcohol before bed can significantly reduce the severity of airway collapses. However, doctors warn that these changes should complement, not replace, professional medical intervention for moderate to severe cases. The goal is to create a comprehensive “heart-sleep” plan that addresses the mechanical causes of apnea while supporting overall vascular health through diet and exercise.
As public awareness grows, the integration of sleep medicine into standard cardiology is becoming the new norm. If you experience persistent morning headaches, excessive daytime sleepiness, or have been told you gasp for air during the night, it may be time to consult a specialist. Addressing a sleep disorder is not just about waking up refreshed; it is a proactive step toward ensuring your heart remains strong and resilient for years to come.