KEY POINTS
- The national surgical waiting list has climbed to 96,000 people, including 11,000 children, with projections suggesting it could reach 160,000 by the end of 2026.
- Medical professionals are earning monthly salaries equivalent to just $14 to $16, forcing many to abandon the healthcare sector for service industry jobs.
- Critical resource scarcities have forced hospital staff to reuse disposable gloves and use plastic water bottles as improvised medical drainage bags.
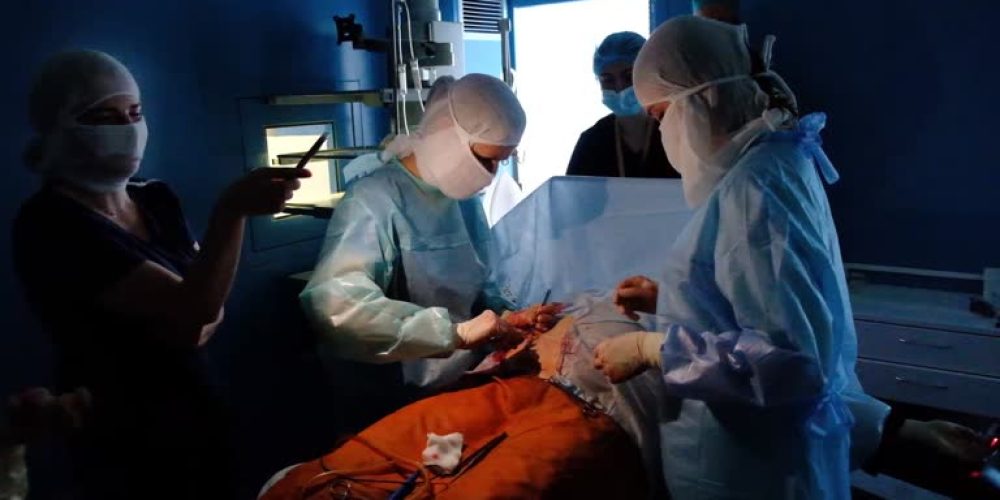
Cuba’s legendary healthcare system, once a primary pillar of the 1959 revolution, is currently facing a catastrophic decline characterized by mass burnout and a near-total lack of basic supplies. Physicians across the island report that the combination of a failing domestic economy and intensified international sanctions has pushed the “Army of White Coats” to a breaking point. Hospitals that were once regional models of excellence now struggle to provide even the most fundamental care due to persistent electrical blackouts and water shortages.
The human toll of this crisis is most visible in the soaring number of delayed procedures. Public Health Ministry data reveals that nearly 100,000 citizens are currently awaiting surgery, a figure expected to grow significantly as the year progresses. In pediatric wards, over 300 operations are postponed weekly because facilities lack essential anesthesia, oxygen, or basic surgical tools. This scarcity has created a desperate environment where nurses in neonatal units are forced to hand-pump ventilators for infants whenever the aging electrical grid fails.
For the doctors themselves, the profession has become a struggle for survival. With state salaries stagnant between 7,000 and 8,000 pesos per month, many highly trained specialists cannot afford basic necessities like eggs or cooking oil. To supplement their income, veteran surgeons are increasingly turning to “side hustles,” such as selling home-cooked meals or working as private house cleaners. The financial disparity is so severe that a single day of waiting tables in the growing private sector can often yield more than a month of government medical pay.
The physical conditions within clinics have deteriorated to unsanitary levels. Due to a lack of industrial cleaning supplies, medical staff frequently bring detergents from their own homes or are forced to scrub floors with nothing but water. Basic items like disposable gloves have vanished from many facilities, and when they are available, they are often washed and reused multiple times. This environment has coincided with a documented rise in infections, which health officials admit is exacerbated by a chronic shortage of antibiotics.
The energy crisis currently gripping the nation has further paralyzed medical delivery. Frequent power outages stop the pumps required to provide running water to primary care clinics, effectively forcing many to halt consultations without making an official public announcement. While the government recently introduced a modest pay increase for overnight shifts, the bonus amounts to only a few cents per hour in real value. These measures have done little to stem the tide of emigration as thousands of healthcare workers flee the island in search of better conditions.
Despite the dire circumstances, high-ranking health officials maintain that the system’s foundation remains intact through the resilience of its staff. The Vice Minister for Public Health recently stated that medical professionals would continue to serve the people regardless of the “difficult circumstances.” However, interviews with frontline workers suggest a growing sense of disillusionment. Many longtime government supporters now admit that their patience is exhausted, though most remain fearful that speaking out publicly could permanently derail their professional careers.
The collapse of the Cuban medical model has profound implications for a country that has long used its healthcare expertise as a tool of global diplomacy. As the waiting lists for cancer treatments and pediatric surgeries continue to expand, the gap between the revolutionary promise of free, world-class care and the daily reality of hospital decay continues to widen. Without a significant influx of resources or a shift in economic policy, the system that once defined the nation’s social contract faces an uncertain future.